The degree of risk from weight loss surgery can depend on the skill of the surgeon.
After sleeve gastrectomy and Roux-en-Y gastric bypass, the third most common bariatric procedure is revision to correct a previous bariatric procedure, as you can see below and at 0:16 in my video Complications of bariatric surgery.
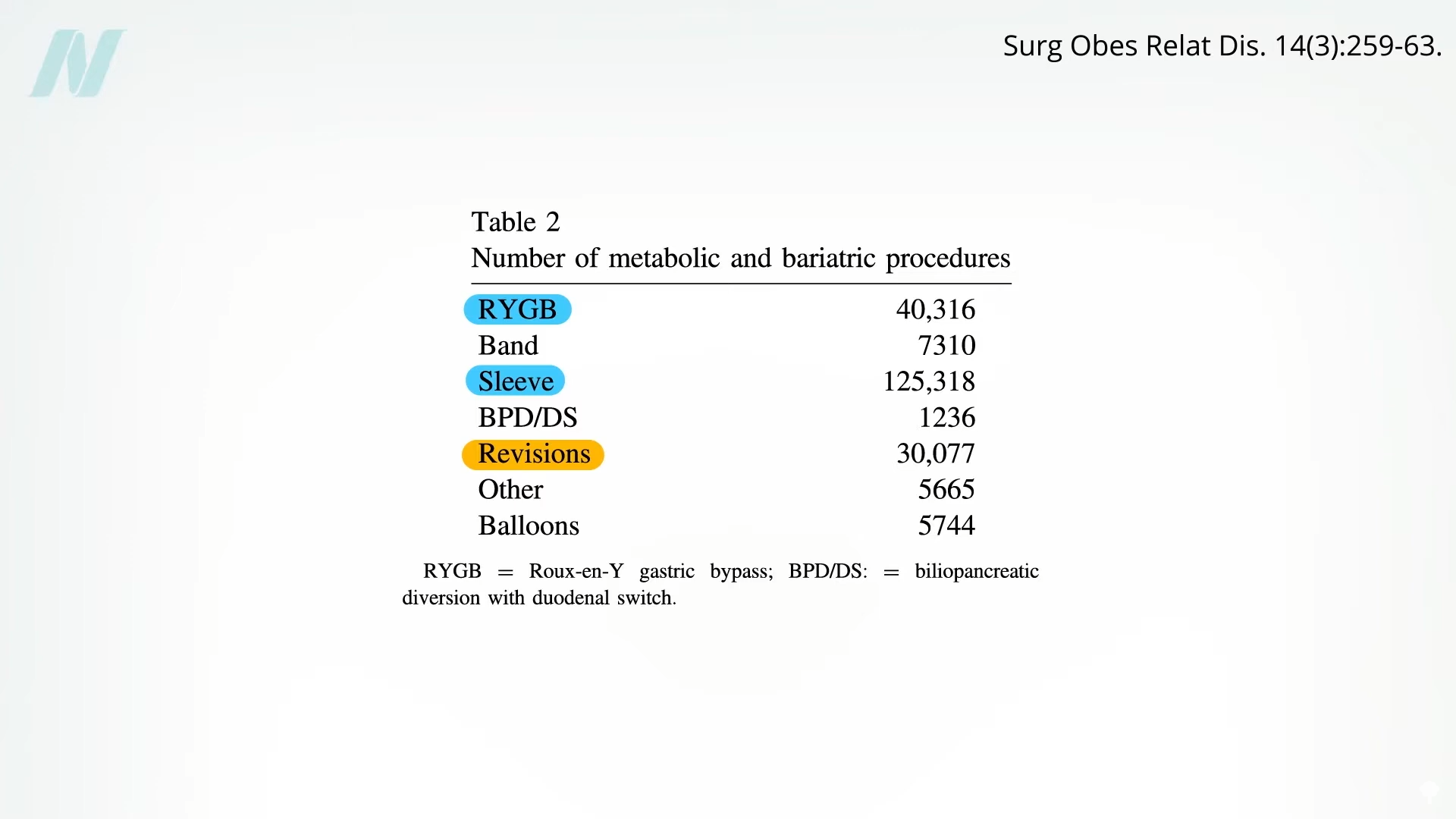

Up to 25% of bariatric patients are obese to go returned to the operating room for complications from the first bariatric surgery. Repeated operations are even more dangerous, with a mortality rate up to 10 times higher, and there is “There is no guarantee of success.” The problem include leaks, fistulas, ulcers, strictures, erosions, obstructions and severe acid reflux.
The level of risk can depends about the skill of the surgeon. In a study conducted in The New England Journal of Medicinebariatric surgeons voluntarily submitted videos of their surgeries to their peer group for evaluation. Technical proficiency varied widely and was associated with rates of complications, rehospitalization, reoperation, and death. Patients operated on by less competent surgeons experienced approximately three times more complications and five times more deaths.
“Some surgeons may be more talented than others, like musicians or athletes” – but practice can make them perfect. Stomach blockage is such a complex procedure that the learning curve can require 500 cases for the surgeon to master the procedure. The risk of complications peaks after about 500 procedures, with the lowest risk among surgeons who have performed more than 600 procedures. The odds of not making it out alive can be double under the knife for those who did less than 75 compared to more than 450, as seen below and at 1:47 in mine. video.

So, if you choose to have surgery, I recommend asking your surgeon how many procedures they have performed and also to choose Accredited Bariatric “Center of Excellence” where operative mortality is two to three times lower than in accredited institutions.
However, the surgeon is not always to blame. In a report titled “The Danger of Broccoli,” a surgeon described a case where a woman went to an all-you-can-eat buffet three months after gastric bypass surgery. She chose really healthy foods – good for her! – but apparently he forgot to chew. His glasses were broken and he ended up in the emergency room, then in the operating room. They cut him open and found “pieces full of broccoli, lima beans and other green leafy vegetables” inside his abdominal cavity. A cautionary tale to be sure, but there’s probably less to say about chewing better after surgery than chewing better before surgery—to keep all of your internal organs healthy in the first place.
Even if the surgical procedure goes Ideally, food replacement and lifelong nutritional monitoring are necessary to avoid vitamin and mineral deficiencies. We to talk about more than anemia, osteoporosis or hair loss. Such defects can be reason complete cases of life-threatening deficiencies such as vitamin deficiency, pellagra, kwashiorkor, and nerve damage that can reveal as loss of vision years or even decades after surgery in case of copper deficiency. Unfortunately, in the reported cases of severe deficiency of vitamin B called thiamine, about one in three patients went ahead to permanent brain damage before the condition takes hold.
Absorption of nutrients is intentional for procedures such as gastric bypass. By cutting segments of the intestines, you can successfully disrupt the absorption of calories – by disrupting the absorption of necessary nutrients. Even people who are alone pass Restrictive procedures such as gastric stapling can be at risk of life-threatening nutrient deficiencies due to persistent vomiting. Vomiting is reported up to 60% of patients after bariatric surgery due to “unwanted eating behaviors”. (In other words, try to eat normally.) Vomiting can help with weight loss, just as the drug for alcoholism called Antabuse can. is used to make them so sick after drinking that they finally learn their lesson.
The “dumping syndrome” can work the same way. A large percentage of gastric bypass patients can to suffer from stomach pain, diarrhea, nausea, bloating, fatigue, or heartburn after eating foods high in calories because they bypass your stomach and go straight to your intestines. As the surgeons describe it, this is a feature, not a bug: “Dumping syndrome is an expected and desired part of the behavioral changes caused by gastric bypass surgery; it can prevent patients from consuming fortified foods.
Dr.’s comment
This is the second in a four-part bariatric surgery series. If you missed the first one, check it out Mortality from weight-loss bariatric surgery.
In the future: Bariatric surgery versus diet to reverse diabetes and How sustainable is weight loss after bariatric surgery?.
My book How not to diet focused only on sustainable weight loss. Check it out at your local library or wherever you get your books. (All proceeds from my books go to charity.)